Everything You Need to Know About Demodex Blepharitis and How to Treat It
Your eyes and eyelids are always red and irritated. What’s up with that?
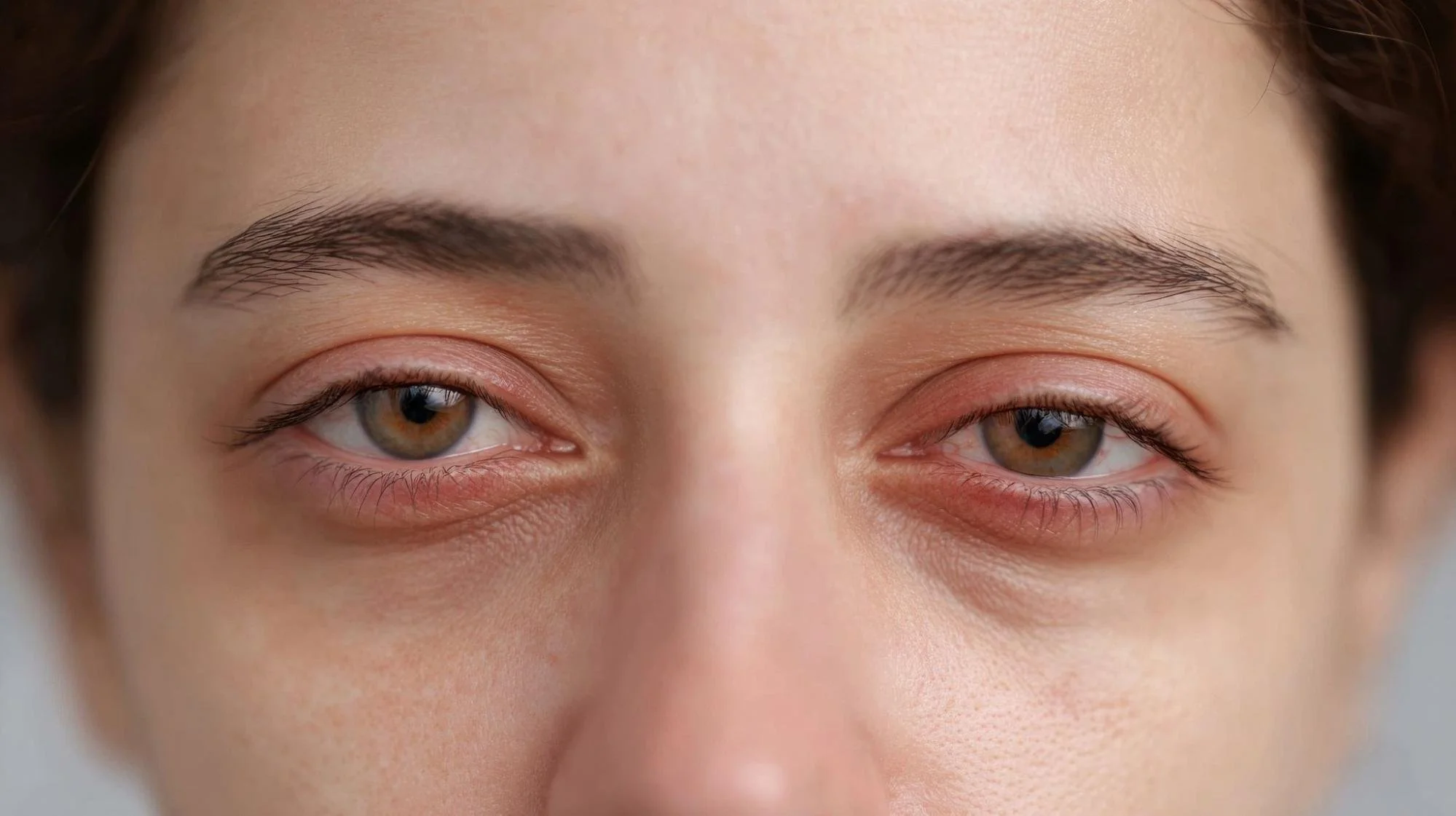
Red, irritated eyes, along with red, swollen, irritated eyelids could be a condition known as blepharitis.
Blepharitis is a chronic (happens over a long period of time or it just keeps recurring) inflammation of the eyelid skin, eyelash follicles, and meibomian glands (eyelid glands that produce an oily substance to keep the tears from evaporating too quickly).
These symptoms can be caused by other issues, but blepharitis is a common reason.
A patient who recently came into the office with blepharitis was initially treated for allergies: Her eyelids were swollen and her eyes were red and itchy. She often felt like she had dirt or some kind of debris in her eyes (this is called a “foreign body sensation"). There were usually dandruff-like flakes along her eyelashes, and her eyelids were sometimes stuck together in the morning.
“How did I get blepharitis? I thought I just had allergies.”
Blepharitis can be caused by excess bacteria, but also be triggered by allergies.
If the problem is excess bacteria, then antibiotics can be prescribed as an eyedrop, ointment, or sometimes an oral tablet. Ocular hygiene is often recommended and includes the application of hot (not so hot that you’re going to scald yourself) compresses for about 10-15 minutes, followed by eyelid massages that help to clear clogged meibomian glands.
Allergies cause blepharitis when our eyes react to cosmetics (make sure that makeup is appropriately removed from around the eyelids and surrounding skin), contact lens solutions, or environmental triggers like pollen and pet dander.
For both bacteria and allergy-related blepharitis, Ocusoft Eyelid Cleansers are a good choice for treatment. There are several types that can be used for blepharitis, allergies and dry eye.
“But if it’s not just basic blepharitis, what else could it be?”
You could be infested with ectoparasitic mites called Demodex.
Little bugs (known as mites) that live on your body all of your life.
Right now, they are on your skin – in your pores.
They reside mostly on your face and, unfortunately, on your eyelids.
When you are awake and going about your daily activities, they like to nuzzle inside the eyelash follicles and meibomian glands.
At night – ahh…at night – they creep out of their lair in order to feed, mate, and make your life as miserable as possible when there is an overgrowth in their population.
“Let me get this straight: There are creepy alien creatures living around my eyes called Demodex? What the hell is Demodex?”
Demodex mites are microscopic microflora (bacteria, viruses, fungi and parasites) living on or within the human body (gut flora) or plants. They can play a vital role in health, immunity, digestion, nutrient synthesis, and can even influence mood and skin health. It’s only when there is an overgrowth of the little beasties that we get a persistent itch (especially in the morning), burning, foreign body sensation, crusted eyelids, and loss of lashes. Some patients have no symptoms at all.
Since they have three body segments, they are considered arthropods. They are graced with four pairs of legs that end with claws.
Their mouths have tiny pincers in which to attach to your eyelashes. Oh, and they burrow into your eyelid glands and eyelash follicles. Yummy.
Demodex mate within the lash follicle opening and lay their eggs inside the follicle or sebaceous gland. Larvae hatch three to four days later and develop into adults within seven days. Their lifecycle is approximately 14 days, and their total lifespan is two to three weeks – the dead mites are left to decompose inside the follicle or sebaceous gland.
A little bit of history:
Demodex mites were first identified and described by the German dermatologist Gustav Simon in 1842. Simon found the mites in hair follicles and called them Acarus folliculorum. Anatomist Jakob Henle recorded them in 1841, and the genus name Demodex was created in 1843 by Richard Owen.
Bringing it all together: “How does Demodex cause blepharitis?”
There are about 65 species of Demodex, but only two, Demodex folliculorum and Demodex brevis, are responsible for Demodex blepharitis (DB).
Demodexfolliculorum are typically 0.30mm to 0.40mm in length and found in clusters around the lash root and lash follicle. They feed on sebum and follicular epithelial cells.
Demodexbrevis is slightly smaller at 0.15mm to 0.20mm in length and travels alone, preferring to infest the meibomian glands (the glands that produce a secretion to keep the tears from evaporating too quickly).
Demodex carry bacteria within their gut which is released when they poop and when they die, as well as harboring bacteria on their surface. Bacteria from either of these sources leads to infection. Hypersensitivity to the proteins that are carried within the mites’ debris and waste causes inflammation.
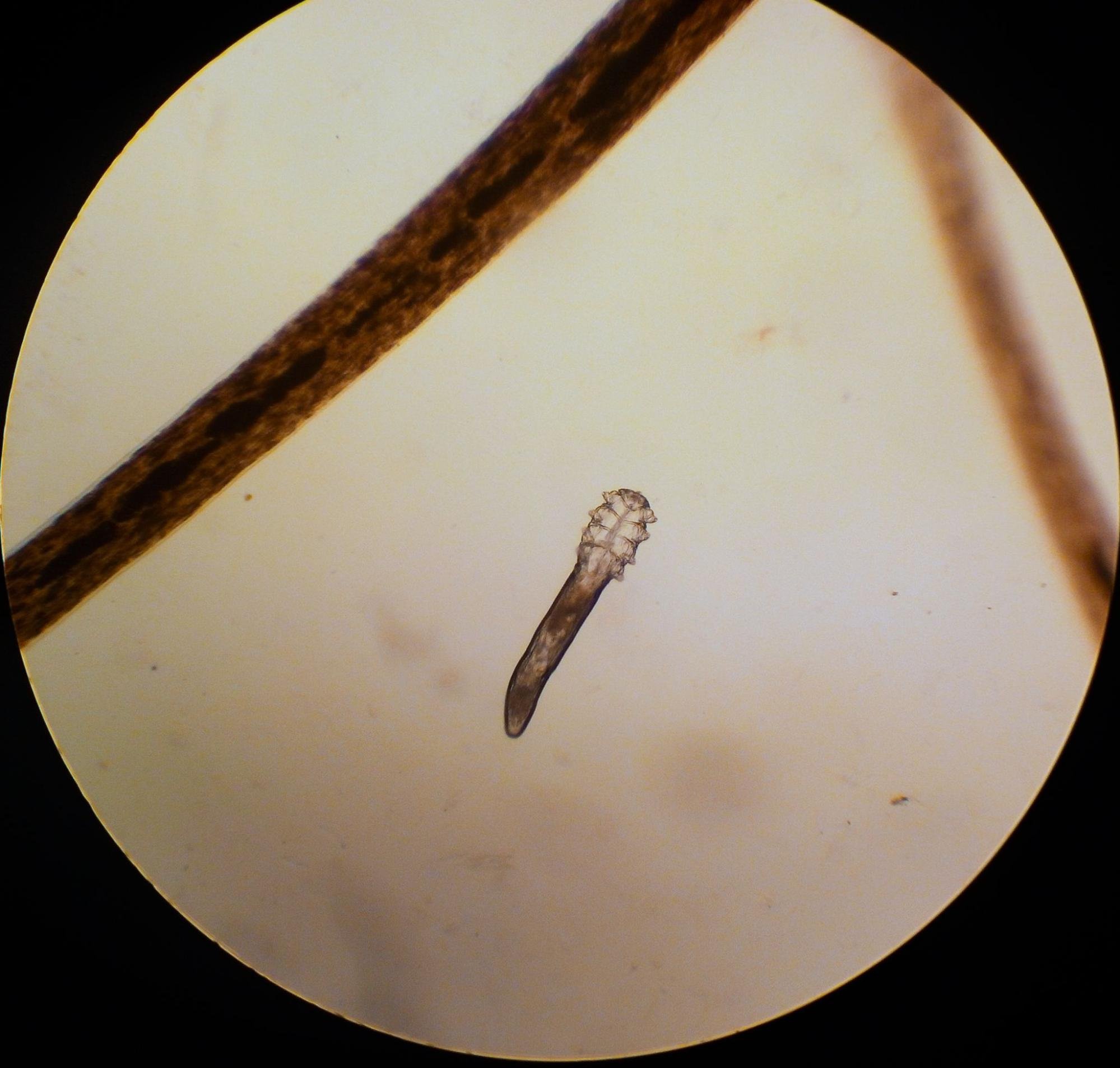
Demodex mite next to an eyelash under a microscope
Wanna see one in action? Just click on this link:
Demodex brevis moving on eye lash
How do you know if you might have the mighty mites?
As previously mentioned, the symptoms of Demodex include persistent itch (especially in the morning), burning, foreign body sensation, crusted eyelids, and loss of lashes. You can also add sticky eyelids, and of course some patients are asymptomatic.
If you recall, the patient above had many symptoms that were alleviated with standard treatment modalities. So why was her newest issue considered DB?
Two reasons:
Her eyes and eyelids ceased to respond to treatment.
But most importantly, because of observations made in the clinic while examining Erica’s eyelashes.
“How does my eye doctor know if it might be the little shits?”
If we rely solely on patient complaints to diagnose DB, it can lead to significant misdiagnosis and lack of effective treatment. So we use an instrument known as a biomicroscope to closely observe your eyelashes for something called “collarettes”.
Collarettes are translucent waxy plugs found at the base of the lashes. They usually signify overpopulation of Demodex. Ok, are you ready for this? Collarettes are composed of regurgitated and undigested material, epithelial cells, keratin, mite eggs and digestive enzymes. Yuck.
First, we ask the patient to look down when examining the lid margin. This can reveal lots of collarettes and misdirected or missing eyelashes.
Next, we inspect the meibomian glands to determine if they are functioning properly. It has been shown in the research that dysfunctional meibomian glands go hand-in-hand with DB.
“Are the bastards contagious?”
Demodex mites are quite common. They can be found on most people in controlled populations that generally don’t cause any trouble.
However, they become more common the older we get and are found more often on diabetics and people with compromised immune systems. It’s generally the overgrowth of the mites that cause symptoms.
Poor hygiene is rarely a reason for an infestation.
Can you go blind from DB?
While permanent blindness is a rare side effect, it is important that the condition be diagnosed and treated in a timely manner.
If left untreated, there is the chance of developing a chronic inflammation of the eyelids. This could lead to styes, meibomian gland problems, chalazions (a lump inside the eyelid due to a previous meibomian infection), and dry eye.
“How do we destroy the damn things? (Please tell me that they can be blasted with a laser!)”
While not a laser, the standard treatment today is to use an eyedrop known as Xdemvy (lotilaner ophthalmic solution 0.25%, Tarsus Pharmaceuticals). The drops are prescribed by your eye doctor and requires a six-week course of treatment with a dosage of one drop of the solution in each eye, administered twice daily approximately 12 hours apart.
The most common side effect is temporary stinging or burning upon installation in about 10% of patients. Other side effects such as corneal irritation and eyelid issues are rare.
Since DB can be a chronic condition, there can be another overgrowth of mites with time. Periodic visits to your eye doctor to monitor the condition is recommended.
Maybe you’d rather not go to your eye doctor. Do over-the-counter treatments like tea tree oil work?
Years ago, tea tree oil was commonly recommended. However, it was never very reliable – sometimes it worked, sometimes it didn’t. But the biggest problem was how badly it irritated the eyes. Very uncomfortable.
You’re better off being treated with Xdemvy by your eye doctor.
How do you get rid of the collarettes (Just short of calling a local witch for a magical poultice)?
Warm compresses alone won’t be as effective as a combination of Ocusoft Lid Scrubs and Xdemvy drops.
Are there any other ways to control the buggers?
Xdemvy is the best product for treatment and management of DB. However, to be complete about other available treatment modalities, here’s a brief list:
Immunomodulators
Anything else?
Here are a few in-office remedies that an experienced eye doctor should be able to perform:
In-office debridement (exfoliation)
Also known as Microblepharoexfoliation, this procedure lasts about 6 to 8 minutes. It is a deep clean of the eyelids and lash line, and for some patients it may need to be repeated every 4-6 months. In addition to this in office treatment daily eyelid hygiene is recommended with use of eyelid cleansers and with the use of NuLids (a handheld, rechargeable, at-home device designed to treat chronic dry eye, blepharitis, and Meibomian Gland Dysfunction (MGD) by gently stimulating, exfoliating, and cleaning the eyelids.
Zest (Zocular Eyelid System Treatment)
An alternative to exfoliative treatment, it involves using an okra-based cleansing gel plus manual debridement of the lids and lashes.
Thermal pulsation treatment: Meibomian gland dysfunction is often seen in DB. These in-office procedures that manage MGD by melting any clogged meibum and then expressing the obstructed glands.
Tear film stabilizer
Miebo: Drops that help to stabilize the tear film by forming a protective monolayer over the surface of the tear film. This mimics the function of the lipid layer to prevent tear evaporation.
Neurostimulatory agent
Tyrvaya: A nasal spray that increases tear production by stimulating the parasympathetic pathway via the trigeminal nerve, one of the twelve cranial nerves.
Why do your eyes feel like crap at night and in the morning?
Remember, Demodex are nocturnal creatures. They thrive at night and in the early hours.
Symptoms, such as itching, are worse at night or in the early morning because Demodex mites are most active during these times. They emerge from their lair (the eyelash follicles, meibomian glands) at night to mate and move across the eyelid margins.
You’ve just been diagnosed with DB. Does this mean an end to wearing contact lenses and makeup?
It is generally challenging to wear contact lenses or eye makeup during an active DB infestation.
If you’re able to wear contact lenses comfortably with DB, then you should remove your lenses before instilling the drop of Xdemvy into your eyes. You must wait a minimum of 15 minutes before you reinsert the lenses.
The strong recommendation is to abstain from wearing contact lenses and/or makeup during treatment to avoid irritation or contamination.
So remember…
If you have eyes or eyelids that are:
Persistently itchy (especially in the morning)
Burning
Gritty with a foreign body sensation
Crusty
Losing lashes
A bit sticky
Not responding to a standard treatment regimen…
Get to your eye doctor as soon as possible in order to determine if you have DB.
You’ll be glad you did!